Osteonecrosis of the jaw in a patient with acute myeloid leukemia, who received azacitidine
Abstract
The first case of osteonecrosis of the jaw (ONJ) related to azacitidine therapy was reported. A 64-year-old male with acute myeloid leukemia, who received 5-azacitidine, presented with pain and purulence of the right second premolar. An unsuccessful endodontic therapy resulted in dental extraction 6 months later. The post-extraction non-healing socket was managed with antibiotics and multiple surgical debridements without response. ONJ stage 2 was diagnosed 12 months after the initial symptoms of pain and purulence and was managed conservatively. Currently the patient is still receiving 5-azacitidine therapy, while ONJ remains asymptomatic. This case highlights the presence of alveolar bone disease prior to the appearance of ONJ. Osteonecrosis in chemotherapy, although rare, may increase as long-term survival of cancer patients, who receive those medications increases. Health care professionals need to be alert, while collaboration with an experienced oral/dental oncologist would be beneficial to the patient.
Keywords
Introduction
Osteonecrosis of the jaw (ONJ) in cancer patients is related to antiresorptive therapy, such as bisphosphonates and denosumab, and angiogenesis inhibitors, such as bevacizumab and sunitinib.[1-3] Medications with antiangiogenic effect, such as sorafenib, imatinib, everolimus, aflibercept, trastuzumab and pazopanib were related to ONJ in few case reports.[4-8] Ipilimumab, a monoclonal antibody against cytotoxic T-Lymphocyte-Associated Antigen-4 (CTLA-4) was recently associated with ONJ.[9] In patients receiving antiresorptives, concurrent chemotherapy was reported as a risk factor, while chemotherapy alone has also been related to ONJ in three patients.[10-12]
Dental extraction has been considered as one of the causes for ONJ.[13-15] This myth has, however, been questioned.[16] It is now believed that the dental extraction, indicated due to periodontal/dental infection and disease, will lead to exposure of the alveolar bone, which may already be necrotic and will not heal.[17] Infection, within a unifying concept of medication-related impaired immune response was proposed to play an important role in the pathophysiology of ONJ.[18]
In this paper we report what we believe is the first case of ONJ in a patient with acute myeloid leukemia (AML), who was treated with azacitidine. The presence of alveolar bone disease leads to the dental extraction and the subsequent diagnosis of ONJ.
Case report
A 64-year-old male, smoker was diagnosed on April 2010 with myelodysplastic syndrome (refractory anemia) of low-risk according to IPSS (normal karyotype, without cytopenia, blasts 3-4%).[19] One year later the patient progressed to refractory anemia with excess blasts, type II (RAEB-II), normal karyotype, without cytopenia, blasts 15%.[20] He was placed on 5-azacitidine therapy [75 mg/m2 (150 mg) day 1 to day 7 on 28 days cycle] with partial remission (Hgb > 11 g/dL, Platelets > 100 × 109/L, Neutrophils > 1.0 × 109/L, bone marrow blasts decreased by 50% but still > 5%). Two years later, after 17 cycles of 5-azacitidine, he progressed to AML. His complete blood counts showed: Hemoglobin 9.6 gr/dL, white blood cells 21.6 × 109/L, absolute neutrofil count of 4.0 × 109/L, immature white blood cells (myelocytes, metamyelocytes) and blasts 5.0 × 109/L, platelets 142.0 × 109/L. Bone marrow biopsy revealed 25-30% infiltration of CD34 (+) cells (blasts). Cytogenetic analysis (karyotype) was normal (46XY). He received 7 + 3 induction chemotherapy [intravenous infusion of Cytarabine (200 mg/m2 day 1 through day 7) and Idarubicin 10 mg/m2 on 30’ infusion on day 2, 4, 6]. During hospitalization the patient developed neutropenic fever, managed with empiric antibiotic treatment (piperacilin + tazobactam and amikacin) and red blood cell and platelets transfusions. Two months later, bone marrow aspiration and flow cytometry disclosed persistent disease.
Patient did not consent to receive induction chemotherapy and was placed on low intensity chemotherapy with hydroxyurea per os for six months. Bone marrow biopsy revealed greater than 60% blast cell infiltration, with a normal karyotype and patient was treated again with 5-azacitidine from that time to present. Bone marrow blasts dropped to 14%.
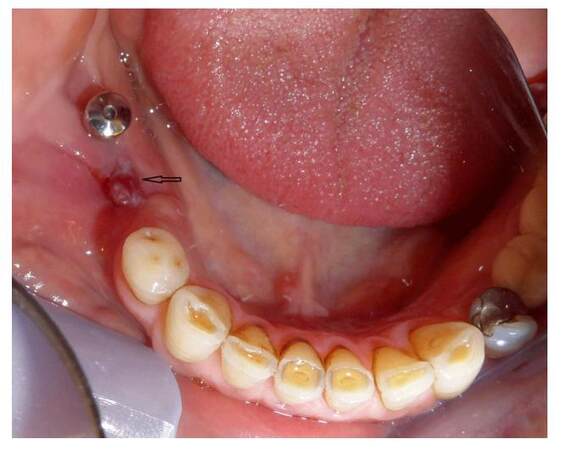
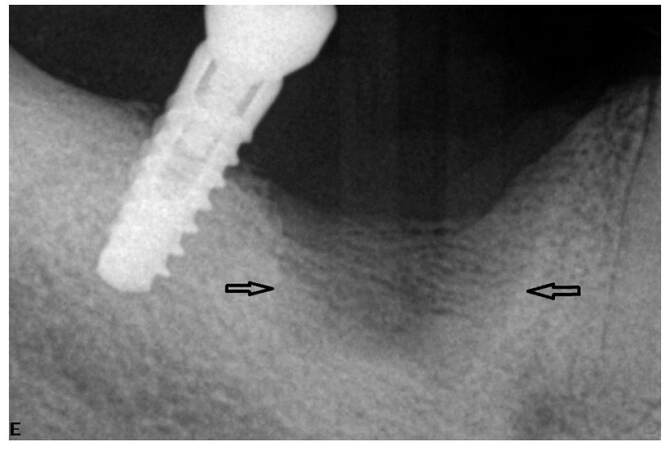
On June 2014 the patient received a restoration of the 2nd right mandibular premolar because of pain. Pain and purulence persisted in spite of endodontic therapy. Dental extraction was recommended and completed in December 2014. The post-extraction follow up revealed a non-healing socket. This area was managed with antibiotics (amoxicillin alone or combined with metronidazole) and surgical debridements (January to July 2015). A biopsy taken from the soft tissue of the socket showed granulation tissue. On July 2015 pain, swelling and purulence at the site of previous extraction [Figure 1], with necrotic bone being probed through a fistula and radiolucency, was observed on the periapical X-ray [Figure 2], leading to the diagnosis of osteonecrosis.
Figure 1. Swelling, fistula and purulunce on the post extraction non-healing socket (July 2015). Necrotic bone could be probed through the fistula
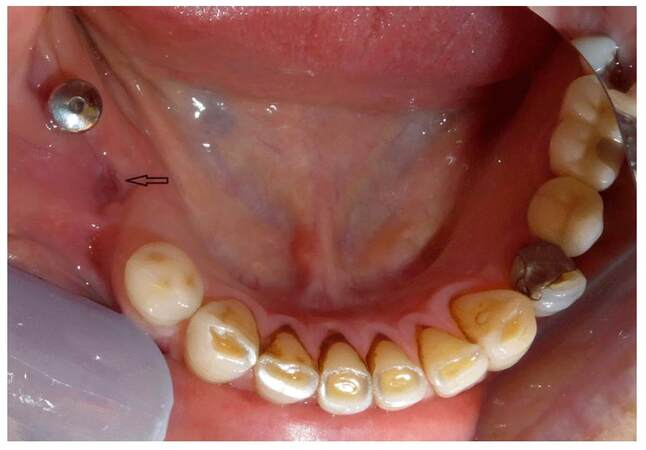
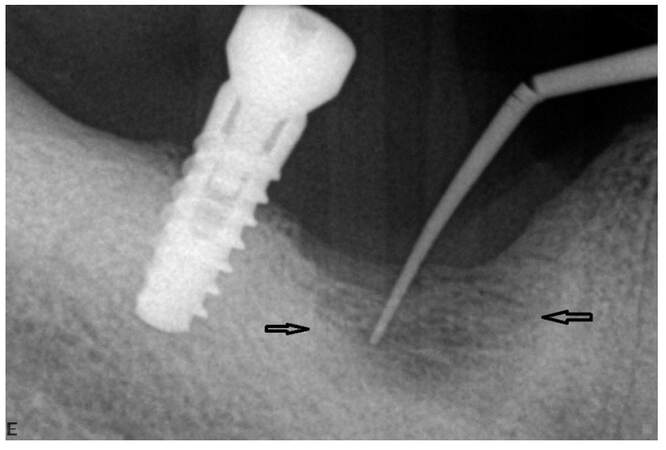
Management with antibiotics, ozone oil applications and low level laser therapy (LLLT) treatments [Ripamonti-11, Nicolatou-13], twice weekly, resulted in remission of symptoms [Figure 3], while the radiolucency and fistula persisted [Figure 4].This is a retrospective case presentation from existing de-identified medical record data. Patient gave consent for the medical record review.
Discussion
Azacitidine is a chemical analogue of the cytosine nucleoside and functions as a DNA demethylating agent and as an antimetabolite.[21] Reduced cell division and growth may result from demethylation of DNA. Azacytidine, as a metabolite, can exert a direct myelotoxic and cytotoxic effect. Azacytidine, by both its demethylating and antimetabolite actions, might have negatively affected the increased need of cellular division and growth of bone remodeling and the soft tissue healing after the dental extraction in our patient. Azacitidine-related cytotoxicity and impaired immune response to infection could have also contributed to the development of alveolar bone disease and infection, which had preceded the appearance of ONJ.
Gemcitabine chemotherapy was associated with ONJ in a patient to Sezary syndrome, an aggressive leukemic form of cutaneous T-cell lymphoma.[12] In that case, ONJ was related to the effects of gemcitabine, through suppression of vascular endothelial growth factor. Osteonecrosis was also reported in a patient with AML and in one with breast cancer, who received aggressive chemotherapy. No azacitidine was administered to the above patient with AML. Neutropenia and severe immune suppression were related to the development of ONJ in those cases.[10] The presently reported patient developed ONJ while he was on azacitidine therapy. T-cell-related altered immune response and infection were related with ONJ in another patient, with advanced metastatic melanoma, who received ipilimumab.[9] Pain, purulence and periodontal ligament widening indicating alveolar bone disease and infection preceded the appearance of ONJ in all those cases, including the present case. Our findings support the proposed role of alveolar bone disease and infection in the pathogenesis of ONJ.[17,18]
The major treatment objectives for patients with ONJ are pain and infection control and minimization of ONJ progression. Antibiotics and topical antiseptics combined with ozone oil applications and LLLT are used as best available clinical practice for early ONJ stages.[1,5,17,22] Ozone oil has antimicrobial and healing properties, while LLLT biostimulation can improve healing.[23,24] The patient was managed with antibiotics, amoxicillin and/or metronidazole, ozone oil applications and LLLT. The long delay (12 months) for the diagnosis of ONJ and the multiple unsuccessful dental and surgical interventions, combined with the continued azacitidine therapy, may be related to the persistent ONJ lesion.
In conclusion, this case increased the list of medications that can lead to ONJ and highlighted the importance of the presence of localized alveolar bone infection prior to the appearance of ONJ. The occurrence, though rare, of this potentially serious complication may increase with the long-term survival of cancer patients.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
1. Ruggiero SL, Dodson TB, Fantasia J, Goodday R, Aghaloo T, Mehrotra B, O'Ryan F. Medication-related osteonecrosis of the jaw-204 update. 2014;1-26. Available from: http://www.aaoms.org/docs/position_papers/mronj_position_paper.pdf.
2. Greuter S, Schmid F, Ruhstaller T, Thuerlimann B. Bevacizumab-associated osteonecrosis of the jaw. Ann Oncol 2008;19:2091-2.
3. Nicolatou-Galitis O, Migkou M, Psyrri A, Bamias A, Pectasides D, Economopoulos T, Raber-Durlacher JE, Dimitriadis G, Dimopoulos MA. Gingival bleeding and jaw bone necrosis in patients with metastatic renal cell carcinoma receicing sunitinib: report of 2 cases with clinical implications. Oral Surg Oral Med Oral Pathol Oral Radiol 2012;113:234-8.
4. Kim DW, Jung YS, Park HS, Jung HD. Osteonecrosis of the jaw related to everolimus: a case report. Br J Oral Maxillofacial Surg 2013;5:e302-4.
5. Nicolatou-Galitis O, Razis E, Galiti D, Vardas E, Tzerbos F, Labropoulos S. Osteonecrosis of the jaw in a patient with chronic myelogenous leukemia receiving imatinib - a case report with clinical implications. Forum Clin Oncol 2013;4:29-33.
6. Ponzetti A, Pinta F, Spadi R, Mecca C, Fanchini L, Zanini M, Ciuffreda L, Racca P. Jaw osteonecrosis associated with aflibercept, irinotecan and fluorouracil: attention to oral district. Tumori 2015 Sep 1:0 ; doi: 10.5301/tj.5000405.
7. Pilanci KN, Alco G, Ordu C, Sarsenov D, Celebi F, Erdogan Z, Agacayak F, Ilgun S, Tecimer C, Demir G, Eralp Y, Okkan S, Ozmen V. Is administration of trastuzumab an independent risk factor for developing osteonecrosis of the jaw among metastatic breast cancer patients under zoledronic acid treatment? Medicine 2015;94:e671.
8. Papadopoulou E, Nicolatou-Galitis O, Vardas E, Repoussis P, Ardavanis A, Bafaloukos D, Sgouros J, Christodoulou C, Vaslamatzis M, Linardou H, Ntalakou E, Marioli N, Stefanou D, Syrigos K. Treatment and prevention of osteonecrosis of the jaw associated with medication: 2009-2014. Support Care Cancer 2015;23:S1-388.
9. Owosho AA, Scordo M, Yom SK, Randazzo J, Chapman PB, Huryn JM, Estilo CL. Osteonecrosis of the jaw a new complication related to Ipilimumab. Oral Oncol 2015;51:e100-1.
10. Infante-Cossio P, Lopez-Martin JC, Gonzalez-Cardero E, Martinez-de-Fuentes R, Casas-Fernandez-Tejerina A. Osteonecrosis of the maxilla associated with cancer chemotherapy in patients wearing dentures. J Oral Maxillofac Surg 2012;70:1587-92.
11. Gaudin E, Seidel L, Bacevic M, Rompen E, Lambert F. Occurrence and risk indicators of medication-related osteonecrosis of the jaw after dental extraction: a systematic review and meta-analysis. J Clin Periodontol 2015;42:922-32.
12. DeSesa CR, Appugounder S, Haberland C, Johnson MP. Osteonecrosis of the jaw in association with chemotherapy in the setting of cutaneous T-cell lymphoma. J Oral Maxillofac Surg 2016;74:292-301.
13. Nicolatou-Galitis O, Papadopoulou E, Sarri T, Boziari P, Karayanni A, Kyrtsonis MC, Repousis P, Barbounis V, Migliorati CA. Osteonecrosis of the jaw in oncology patients treated with bisphosphonates: prospective experience of a dental oncology center. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2011;112:195-202.
14. Vardas E, Coward T, Papadopoulou E, Nicolatou-Galitis O. Dental extractions as the major local risk factor of bisphosphonates related jaw osteonecrosis in cancer patients receiving intravenous bisphopshonates therapy. A systematic review. Mediterr Oncol J MOJ 2014;1:26-33.
15. Yazdi PM, Schiodt M. Dentoalveolar trauma and minor trauma as precipitating fcators for medication-related osteonecrosis of the jaw (ONJ): a retrospective study of 149 consecutive patients from the Copenhagen ONJ Cohort. Oral Surg Oral Med Oral Pathol Oral Radiol 2015;119:416-22.
16. Migliorati CA. Dispelling the myths asscociated with osteonecrosis of the jaw. ASCO Post 2015;6:Issue 15.
17. Nicolatou-Galitis O, Razis E, Galiti D, Galitis E, Labropoulos S, Tsimpidakis A, Sgouros J, Karampeazis A, Migliorati C. Periodontal disease preceding osteonecrosis of the jaw (ONJ) in cancer patients receiving antiresorptives alone or combined with targeted therapies: report of 5 cases and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol 2015;120:699-706.
18. Katsarelis H, Shah NP, Dhariwal DK, Pazianas M. Infection and medication-related osteonecrosis of the jaw. J Dent Res 2015;94:534-9.
19. Greenberg P, Cox C, LeBeau MM, Fenaux P, Morel P, Sanz G, Sanz M, Vallespi T, Hamblin T, Oscier D, Ohyashiki K, Toyama K, Aul C, Mufti G, Bennett J. International scoring system for evaluating prognosis in myelodysplastic syndromes. Blood 1997;89:2079-88.
20. Swerdlow SH, Campo E, Harris NL, Jaffe ES, Pileri SA, Stein H, Thiele J, Vardiman JW. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC; 2008:87-107.
21. . http://chemocare.com/chemotherapy/drug-info/Vidaza.aspx. Downloaded: January 2, 2016
22. Ripamonti C, Cislaghi E, Mariani L, Maniezzo M. Efficacy and safety of medical ozone (O3) delivered in oil suspension applications for the treatment of osteonecrosis of the jaw in patients with bone metastases treated with bisphopshonates: Preliminary results of a phase I-II study. Oral Oncol 2011;47:185-90.
23. Vesconi P, Giovannacci I, Merigo E, Meleti M, Manfredi M, Formaini C, Namour S. Tooth extractions in high-risk patients under bisphosphonate therapy and previously affected with osteonecrosis of the jaws: surgical protocol supported by low-level Laser therapy. J Craniofac Surg 2015;26:696-9.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Nicolatou-Galitis O, Galiti D, Moschogianni M, Sachanas S, Edwards BJ, Migliorati CA, Pangalis G. Osteonecrosis of the jaw in a patient with acute myeloid leukemia, who received azacitidine. J Cancer Metastasis Treat 2016;2:220-3. http://dx.doi.org/10.20517/2394-4722.2016.06
AMA Style
Nicolatou-Galitis O, Galiti D, Moschogianni M, Sachanas S, Edwards BJ, Migliorati CA, Pangalis G. Osteonecrosis of the jaw in a patient with acute myeloid leukemia, who received azacitidine. Journal of Cancer Metastasis and Treatment. 2016; 2: 220-3. http://dx.doi.org/10.20517/2394-4722.2016.06
Chicago/Turabian Style
Nicolatou-Galitis, Ourania, Dimitra Galiti, Maria Moschogianni, Sotirios Sachanas, Beatrice J. Edwards, Cesar A. Migliorati, Gerassimos Pangalis. 2016. "Osteonecrosis of the jaw in a patient with acute myeloid leukemia, who received azacitidine" Journal of Cancer Metastasis and Treatment. 2: 220-3. http://dx.doi.org/10.20517/2394-4722.2016.06
ACS Style
Nicolatou-Galitis, O.; Galiti D.; Moschogianni M.; Sachanas S.; Edwards BJ.; Migliorati CA.; Pangalis G. Osteonecrosis of the jaw in a patient with acute myeloid leukemia, who received azacitidine. J. Cancer. Metastasis. Treat. 2016, 2, 220-3. http://dx.doi.org/10.20517/2394-4722.2016.06
About This Article
Copyright
Author Biographies

Data & Comments
Data
 Cite This Article 6 clicks
Cite This Article 6 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.