EGFR mutation -- a commonly neglected mutation in squamous cell lung carcinoma
Abstract
Lung cancer is the leading cause of cancer-related death worldwide. Advances in molecular biology have unveiled various targetable mutations with epidermal growth factor receptor (EGFR) being most common. EGFR testing is recommended for all locally advanced or metastatic adenocarcinoma lungs but recommendation in squamous histology is uncertain. However, just on the basis of histology, EGFR testing should not be withheld in patients diagnosed as squamous cell cancer on small biopsy, in females, never smokers and Asians. We report two cases with squamous cell lung cancer diagnosed on small biopsy, in non smoker females with EGFR mutations emphasizing the importance of testing in such population.
Keywords
Introduction
Lung cancer is the most common cancer in the world accounting for 12.9% of total cases and 19.4% of total cancer related mortality.[1] Advances in molecular biology have led to the identification of mutations within the epidermal growth factor receptor (EGFR), and the finding that these mutations make tumors exquisitely sensitive to EGFR tyrosine kinase inhibitors (TKIs), has revolutionized treatment of non-small cell lung cancer (NSCLC). EGFR mutations are more common in never-smokers, in patients with Asian ethnicity, and in patients with adenocarcinoma histology.[2] However, solely on the basis of histology, EGFR testing should not be excluded in patients with squamous cell cancer, especially females, never smokers, Asian ethinicity and squamous histology diagnosed on small biopsy as adenocarcinomatous component cannot be ruled out on small biopsy specimens.[3] We present two cases of squamous cell lung cancer diagnosed on small biopsy in non smoker females with EGFR mutations who benefitted with oral TKIs.
Case report
Case 1
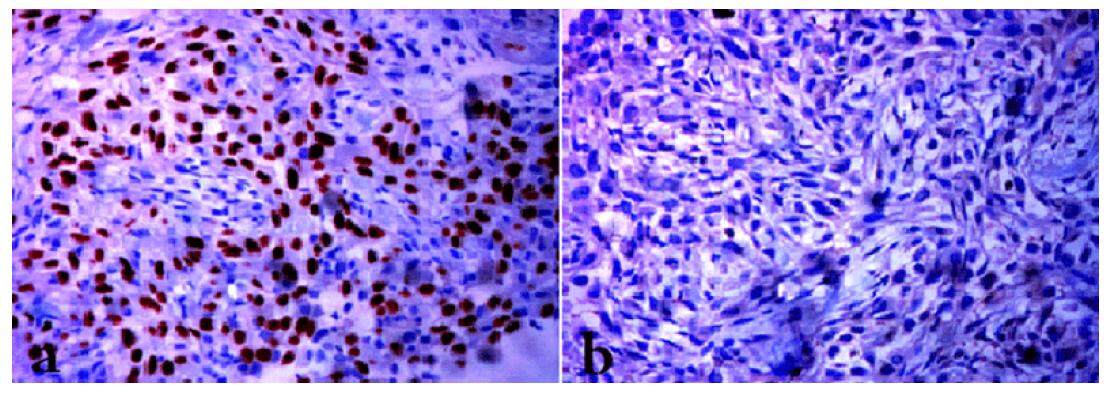
A 56-year-old female, diabetic, hypertensive, non smoker presented with history of cough, weight loss and right sided weakness. Magnetic resonance imaging brain showed two hypodense lesions in left frontal lobe. Positron emission tomography-computed tomography revealed right lung mass with mediastinal lymph nodes, brain, adrenal, pancreatic and bone lesions. A core needle biopsy from lung mass revealed squamous cell carcinoma, p40 positive and thyroid transcription factor (TTF) negative [Figure 1]. In view of symptomatic brain metastasis, she was treated with whole brain radiotherapy followed by two cycles of gemcitabine and carboplatin based chemotherapy. However, in view of poor tolerability due to grade 4 neutropenia and poor performance status, chemotherapy could not be given. Her biopsy was reassessed for EGFR mutational analysis and showed L858R mutation positive. She was started on erlotinib and imaging studies after 2 months of therapy demonstrated significant tumor response in the pulmonary lesions and in the metastatic sites.
Case 2
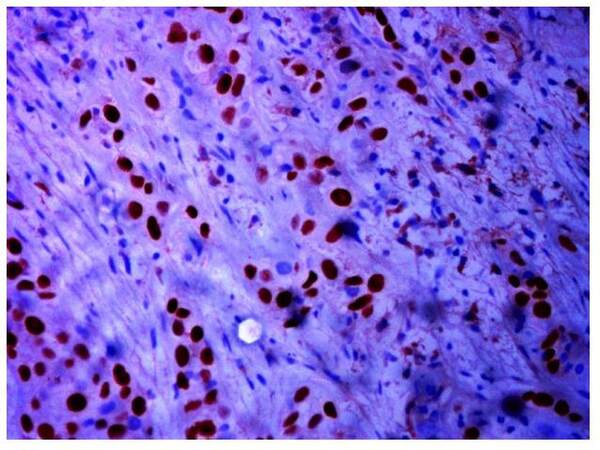
A 44-year-old female, diabetic, hypertensive, non smoker presented with history of breathlessness. Bronchoscopy showed malignant intermediate bronchus obstruction. Bronchial biopsy revealed squamous cell carcinoma expresses p40 [Figure 2] but negative for TTF1. In view of her being non smoker EGFR mutation was tested and was positive for exon 21L858R mutation. After 3 cycles of gemcitabine and cisplatin based chemotherapy there was partial response and now she was on maintenance erlotinib with good disease control.
Discussion
Deeper understanding of the pathobiology of NSCLC has led to the development of small molecules that target genetic mutations known to play critical roles in the progression to metastatic disease. EGFR mutation is one of the most common targetable mutations in NSCLC particularly in non squamous histology. The incidence of EGFR mutations in NSCLC varies by ethnicity, with studies estimating a range from 10-15% of Caucasians to 40-50% of Asians.[4] In India the frequency of EGFR mutations has been found to be between 25-40% in various studies.[5] However, EGFR mutation occurs only in less than 5% patients of squamous cell histology. We present two cases of squamous cell carcinoma of lung with activating EGFR mutation. Thus, just on the basis of histology, patient should not be deprived of potentially beneficial non toxic therapies and can derive same benefits with oral TKIs as in patients of adenocarcinoma histology,[6] especially in light of some important caveats regarding exclusion of testing in all cases diagnosed as squamous cell carcinoma. First, a small biopsy sample showing squamous morphology does not exclude the possibility of an adenocarcinomatous component elsewhere in the lesion. Second, the distinction between adenocarcinoma and squamous cell carcinoma can be extremely challenging in some cases.[7] EGFR mutations have been found to be more common in female patients, never-smokers, and patients of Asian ethnicity irrespective of histology. In conclusion, EGFR testing should be tested in patients with squamous cell lung cancer, especially in females, never smokers, Asian ethnicity and squamous histology diagnosed on small biopsy.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
REFERENCES
1. Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, Rebelo M, Parkin DM, Forman D, Bray F. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 2015;136:E359-86.
2. Rosell R, Moran T, Queralt C, Porta R, Cardenal F, Camps C, Majem M, Lopez-Vivanco G, Isla D, Provencio M, Insa A, Massuti B, Gonzalez-Larriba JL, Paz-Ares L, Bover I, Garcia-Campelo R, Moreno MA, Catot S, Rolfo C, Reguart N, Palmero R, Sánchez JM, Bastus R, Mayo C, Bertran-Alamillo J, Molina MA, Sanchez JJ, Taron M; Spanish Lung Cancer Group. Screening for epidermal growth factor receptor mutations in lung cancer. N Engl J Med 2009;361:958-67.
3. Kang SM, Kang HJ, Shin JH, Kim H, Shin DH, Kim SK, Kim JH, Chung KY, Kim SK, Chang J. Identical epidermal growth factor receptor mutations in adenocarcinomatous and squamous cell carcinomatous components of adenosquamous carcinoma of the lung. Cancer 2007;109:581-7.
4. Mitsudomi T, Yatabe Y. Epidermal growth factor receptor in relation to tumor development: EGFR gene and cancer. FEBS J 2010;277:301-8.
5. Malik PS, Raina V. Lung cancer: prevalent trends and emerging concepts. Indian J Med Res 2015;141:5-7.
6. Xu J, Chu T, Jin B, Dong X, Lou Y, Zhang X, Wang H, Zhong H, Shi C, Gu A, Xiong L, Zhao Y, Jiang L, Zhang J, Han B. Epidermal growth factor receptor tyrosine kinase inhibitors in advanced squamous cell lung cancer. Clin Lung Cancer 2016;17:309-14.
7. Thunnissen E, Kerr KM, Herth FJ, Lantuejoul S, Papotti M, Rintoul RC, Rossi G, Skov BG, Weynand B, Bubendorf L, Katrien G, Johansson L, López-Ríos F, Ninane V, Olszewski W, Popper H, Jaume S, Schnabel P, Thiberville L, Laenger F. The challenge of NSCLC diagnosis and predictive analysis on small samples. Practical approach of a working group. Lung Cancer 2012;76:1-18.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Saini R, Batra U, Jain A, Agrawal C. EGFR mutation -- a commonly neglected mutation in squamous cell lung carcinoma. J Cancer Metastasis Treat 2016;2:253-4. http://dx.doi.org/10.20517/2394-4722.2016.07
AMA Style
Saini R, Batra U, Jain A, Agrawal C. EGFR mutation -- a commonly neglected mutation in squamous cell lung carcinoma. Journal of Cancer Metastasis and Treatment. 2016; 2: 253-4. http://dx.doi.org/10.20517/2394-4722.2016.07
Chicago/Turabian Style
Saini, Rajeev, Ullas Batra, Akhil Jain, Chaturbhuj Agrawal. 2016. "EGFR mutation -- a commonly neglected mutation in squamous cell lung carcinoma" Journal of Cancer Metastasis and Treatment. 2: 253-4. http://dx.doi.org/10.20517/2394-4722.2016.07
ACS Style
Saini, R.; Batra U.; Jain A.; Agrawal C. EGFR mutation -- a commonly neglected mutation in squamous cell lung carcinoma. J. Cancer. Metastasis. Treat. 2016, 2, 253-4. http://dx.doi.org/10.20517/2394-4722.2016.07
About This Article
Copyright
Data & Comments
Data

 Cite This Article 2 clicks
Cite This Article 2 clicks










Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.