Novel immunotherapeutic approaches in head and neck cancer
Abstract
Unresectable recurrent or metastatic head and neck cancer is an incurable disease with survival of approximately 12 months. Head and neck tumors exhibit numerous derangements in the tumor microenvironment that aid in immune evasion and may serve as targets for future therapies. Pembrolizumab is now approved as a first line therapy. Despite the promise of currently approved immunotherapies there continues to be low response rates and additional strategies are needed. Here, alterations in the immune microenvironment and current therapeutic strategies are reviewed with a focus on novel immunologic approaches.
Keywords
Introduction
Head and neck squamous cell carcinoma (HNSCC) represents the 6th most common malignancy globally and accounts for 1%-2% of all cancer related deaths[1]. HNSCC is comprised of a heterogenous group of tumors including those arising from the oral cavity, oropharynx, hypopharynx and larynx. Traditional risk factors include tobacco, alcohol, and more recently human papillomavirus (HPV). High risk strains of HPV (HPV 16, 18) now are responsible for 70%-80% of oropharyngeal squamous cell carcinoma[2,3].
Treatment of HNSCC varies by tumor site and stage, however the mainstays of treatment include surgery, radiation, and cytotoxic chemotherapy. Despite advancements in surgical and radiation techniques, treatment failures occur in up to 50% of patients with HNSCC[4,5]. In the unresectable recurrent or metastatic (R/M) setting, chemotherapy has previously been the main therapeutic option, with dismal outcomes and median survival times ranging from 6-10 months[6]. Immunotherapy, particularly checkpoint inhibitors, have shown promising results in R/M HNSCC[7,8]. In June of 2019, the United States Food and Drug Administration approved pembrolizumab as a 1st line treatment for patients based on PD-L1 expression in the tumor immune microenvironment[9]. Despite these recent reports, overall response rates remain low with underwhelming improvements in long term survival. Hence there continues to be a need for novel therapeutic options.
Head and neck tumors display various derangements in anti-tumor immunity and detailed understanding of these changes has led to development of currently approved immunotherapies. Here, we discuss alterations in the tumor immune microenvironment, review the mechanism of current treatments and focus on approaches for development of novel immunologic therapies.
Derangement of head and neck tumor immune microenvironment
Tumor immunity cycle
Anti-tumor immunity requires a complex set of interactions between the tumor and host immune system. This process has been termed the cancer immunity cycle[10,11]. Initial tumor cell lysis results in release of tumor specific antigens (TAs) and priming of antigen presenting cells (APCs). APCs then interact with host immune cells resulting in activation and trafficking of cytoxic T cells (CTLs) into the tumor. Once in the tumor, CTLs identify malignant cells displaying the specified tumor antigen and target them for cell death. Tumor antigens also referred to as neoantigens have become an area of intense research. These can be derived from either driver or passenger mutations and generation of TAs is thought to be closely linked to mutational burden, with a higher mutational load correlating to increased TAs[12,13]. HNSCC has been found to have 1 of highest mutational burdens of all malignancies, likely due to their relationship with carcinogen exposure (i.e., tobacco smoke) which results in significant mutagenesis[13,14]. As sequencing techniques have advanced, more sophisticated modeling has allowed for identification of specific mutational profiles including smoking and APOBEC signatures as well as prediction of neoantigen load[15]. Detailed review of neoantigen prediction modeling has previously been published and is outside the scope of this review[16-19]. Finally, with targeted tumor cell death by CTLs there is further release of tumor antigens resulting in perpetuation of the cycle. Head and neck tumors have evolved multiple mechanisms of immune escape which will be reviewed below in context of the cancer-immunity cycle.
Inhibition of antigen processing and presentation and immune cell activation
While HNSCC is thought to be highly antigenic, further steps are required for activation of a TA-specific adaptive immune response. After being released from tumor cells, TAs are degraded, processed, and presented by professional APCs including dendritic cells. Normal processes allow for extracellular protein presentation through major histocompatibility complex (MHC) class II and CD4 interaction, however, for TA to activate a CD8 response, cross presentation occurs, requiring an additional set of processing machinery[20]. Large scale sequencing studies as well as analysis of TCGA data have revealed that up to 20% of HNSCCs contain alterations in antigen processing machinery (APM) or downregulation of MHC class I[20,21]. In HPV positive tumors, the latter is thought to be mediated through viral oncoproteins, E5 and E7, which have been shown to downregulate both MHC class I and class II[22-24]. Additional studies show that patients with alterations in these pathways had both decreased CD8 T cell infiltration and worse survival outcomes[25,26], indicating inhibition of antigen presentation may play a key role in head and neck tumor immune escape.
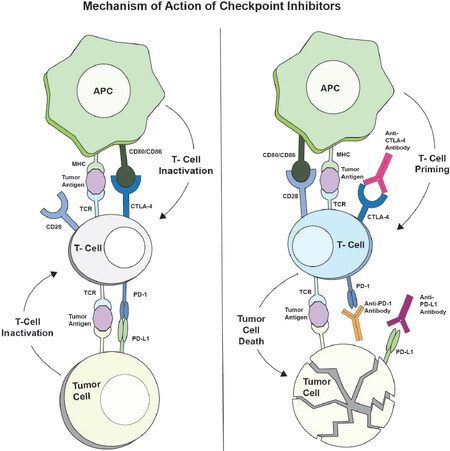
Once primed, APCs interact with and activate CTLs. Activation of CTLs occurs through contact between the T cell receptors and MHC class I bound to TA. This process requires a co-stimulatory signal between CD80 (present on the surface of the APC) and CD28 (a surface receptor on the CTL). Conversely, CD80 may instead bind CTL associated antigen 4 (CTLA-4) leading to CTL inhibition[11,27,28]. While in normal physiologic conditions, the CTLA-4 immune checkpoint prevents an exaggerated immune response, in the setting of malignancies, it is thought to be a major mechanism of immune escape[27,28].
Immune cell trafficking and infiltration
After priming and activation, CTLs infiltrate the tumor where they identify malignant cells displaying the specific TAs. In order for successful immune cell trafficking to occur, there must be appropriate cytokine signaling as well as an optimized physical environment. Physical blockade of immune cell infiltration has been suggested to play a role in immune escape and is thought to be mediated through elevated vascular endothelial growth factor (VEGF) signaling. This results in increased angiogenesis and increased oncotic pressure within the tumor creating a physical barrier to infiltration[29]. In vivo studies evaluating anti-angiogenic tyrosine kinase inhibitors have shown an increase in tumor infiltrating lymphocytes correlating with reduced angiogenesis[30,31]. Tumors may also promote an immune deplete environment through recruitment of suppressive and regulatory immune cells. This is achieved through direct secretion of suppressive cytokines such as tumor growth factor beta (TGF-β), or through secretion of CCL, CXCL, or VEGF which recruit myeloid derived suppressor cells (MDSC)[32-34]. MDSCs are able to directly induce T cell tolerance through arginase, nitric oxide synthase[35] and indoleamine 2,3-dioxygenase (IDO)[36] dependent mechanisms[32,37,38]. In HNSCC, increased tumor lymphocyte infiltration is linked to improved prognosis[39-41], while elevated levels of MDSCs have been linked worse prognosis[38,42].
PD-1/PD-L1 axis inhibition
Once in the tumor, CTLs induce tumor cell death. However, tumor cells may inhibit cell killing via co-stimulatory signals through the PD-1/PD-L1 axis. PD-1 is a member of the CD28 superfamily and is expressed on dendritic cells, regulatory T cells (Treg), CD8 and CD4 T cells, MDSCs, and natural killer cells (NK)[43]. PD-L1 is expressed on APCs and causes T cell anergy and apoptosis upon binding with PD-1 receptors, thereby serving as a check to prevent an overactive immune response[44,45]. However, upregulation of PD-L1 or additional PD-1 ligands such as PD-L2 can also be seen on tumor cells and acts as a mechanism of immune escape in various malignancies[46]. The interaction between PD-L1 and PD-1 is complex and has been previously explored in multiple reviews[47,48]. In HNSCC, PD-1/PDL-1 expression has been reported in 46%-100% of tumors and with higher expression in HPV-positive tumors compared to HPV negative tumors[46,49-51]. Multiple currently approved therapeutics have been developed to target the PD-1/PD-L1 axis, including Pembrolizumab and Nivolumab as well as additional therapeutics that are currently undergoing clinical investigation such as Atezolizumab, and Durvalumab among others [Figure 1]. Both Pembrolizumab and Nivolumab inhibit PD-1, while the latter 2 (Atezolizumab and Durvalumab) target PD-L1. As PD-1 can be activated by additional ligands such as PD-L2 there is a theoretical advantage to targeting PD-1 over PD-L1, however anti-PD-1 and anti-PD-L1 therapies have demonstrated similar response rates and toxicity profiles in clinical trials as discussed below.
Immunomodulatory mechanisms of tradition therapies
Prior to review of current immunotherapeutics, it is prudent to discuss the immunomodulatory role of traditional therapies. Both platinum based chemotherapy and radiation have been shown to alter the tumor immune microenvironment. In vivo studies revealed that cisplatin treatment increases expression of MHC class I and antigen presentation machinery in patient derived HNSCC cell lines[52]. While these changes may improve the anti-tumor immune response, this same study also demonstrated increased PD-L1 expression, decreased IFN-γ release by Tregs, and increased antigen specific T cell death with cisplatin treatment[52,53]. These alterations in the tumor immune microenvironment suggest potential for dual treatment with cisplatin and anti-PD-1/PD-L1 immunotherapeutics, and in vivo studies have shown benefit of combination therapy[52]. While cisplatin leads to increased Treg populations in HNSCC, similar studies performed in other types of malignancies have found that cisplatin treatment can actually lead to decreased Treg function and CTL activation by dendritic cells[53,54]. These contradicting results suggest a complex mechanism by which cisplatin may affect the tumor microenvironment.
Radiation therapy (RT) is commonly used in the treatment of head and neck cancer and has also been shown to play a regulatory role in the tumor immune microenvironment. The specific mechanism by which radiation enhances the immune system is multifactorial. RT has been shown to increase production of TA[55], increase expression of MHC class I and APM components[56-58], and increase the number of tumor infiltrating lymphocytes[59]. Similar to chemotherapy, RT can also suppress the immune response through recruitment of MDSCs and other suppressive immune cells[60]. Further indication of the immunoregulatory effect of radiation is evident by the fact that radiation has been reported to induce tumor cell death in tumor deposits outside of the irradiated field. This is termed the abscopal effect and is thought to be an immune mediated response[61,62].
Mechanisms of currently approved immunotherapeutics
In addition to traditional therapies, there are 3 currently approved biologics for HNSCC including Cetuximab, Pembrolizumab, and Nivolumab, which have also been shown to have immunomodulatory mechanisms.
Cetuximab, a monoclonal antibody against epidermal growth factor receptor (EGFR), was designed as a targeted therapy. However, recent studies have suggested that it may be tumoricidal via immune modulation[63]. Accumulating evidence suggests that cetuximab increases antibody dependent cellular cytotoxicity (ADCC) of NKs[63-65]. As Tregs inhibit NK mediated ADCC, through a TGF-β dependent pathway, it is postulated Cetuximab’s mechanism of action may be through reduction or inhibition of Tregs. A recent study demonstrated a decrease in the number of Treg in peripheral blood samples in HNSCC patients treated with Cetuximab. This observed decrease in Treg population also correlated with improved overall survival in this cohort[63]. Additional mechanisms of cetuximab have also been suggested, including increased crosstalk between dendritic cells and NK cells with further activation of the adaptive immune response, specifically targeting EGFR expressing cells[66,67] and activation of the complement system[68]. More recent studies have also indicated that cetuximab may increase CTLA-4 and PD-1/PD-L1 expression and suggest a need for combination therapies[64,69].
Both Pembrolizumab and Nivolumab which target PD-1 have proven to have clinical benefit in patients with progressive disease after platinum based therapy[7,70]. Initial approval for these drugs occurred in 2016 after the published results from multiple clinical trials were released. The phase III clinical trial, CHECKMATE-141, evaluated nivolumab vs. standard of care (SOC) chemotherapy in patients with platinum refractory R/M HNSCC. The overall response rate (ORR) for the nivolumab group was 13.3% compared to 5.5% in the SOC arm. Furthermore, nivolumab demonstrated an improved survival [7.5 months vs. 5.1 months (HR = 0.7, 97.7%CI: 0.51-0.96)] which was the 1st time a 2nd line agent demonstrated survival benefit[7]. Similar results were seen in the KEYNOTE 040 trial, comparing Pembrolizumab to SOC in patients with R/M HNSCC who had failed platinum therapy. In this trial there was an ORR of 14.6% in the pembrolizumab group compared to 10.1% in the SOC group and a median OS of 8.4 months vs. 6.9 months (95%CI: 0.65-0.98)[70]. Both studies had secondary endpoints evaluating survival outcomes stratified by PD-L1 status and revealed a greater benefit in patients with positive PD-L1 expression although not statistically significant. These results supported the use of nivolumab or pembrolizumab as a standard of care treatment for patients with platinum refractor R/M HNSCC.
Until recently, there has been no data supporting use of PD-1 inhibitors as a first line treatment option for R/M HNSCC. The results of the KEYNOTE 048 trial were presented at the 2019 American Society of Clinical Oncology meeting[71]. This study evaluated the use of pembrolizumab alone, pembrolizumab with platinum and fluorouracil, vs. the EXTREME regimen in patients with R/M HNSCC. Results revealed an improvement in OS in all patients treated with pembrolizumab with a PD-L1 combined positive score ≥ 1% by the 22C3 assay[9].
While there are no mature data evaluating the effect of anti-PD-L1 therapeutics, such as Atezolizumab or Durvalumab, ongoing phase I and II trials have demonstrated excellent safety profiles with promising responses. A phase I trial published by Colevas et al.[72] in 2018 enrolled 32 patients with advanced unresectable or incurable HNSCC who underwent treatment with Atezolizumab. The overall response rate in this cohort was 22% with a median progression free survival of 2.6 months and median overall survival of 6 months. Responses were found to be independent of PD-L1 expression level or HPV status. While 66% of patients experienced treatment related adverse events, only 4 patients (13%) had grade 3 or 4 toxicity. Given these results, a phase III randomized control trial is currently underway investigating the use of Atezolizumab in HNSCC (NCT03452137). Durvalumab has also been evaluated in Phase I/II trials in HNSCC. A study by Segal et al.[73] published in 2019 examined 62 patients with unresectable and previously treated HNSCC treated with Durvalumab and found an ORR of 6.5% with a median overall survival of 8.4 months. Unfortunately, the results of the phase III EAGLE trial evaluating Durvalumab as single modality therapy in patients with progressive disease after platinum therapy was did not reveal any survival benefit alone or in combination with CTLA-4 inhibitor, Tremelimumab[74]. An ongoing trial (NCT02551159) is evaluating Durvalumab with and without Tremelimumab in patients with R/M disease who have not received previous treatment for recurrent disease. A summary of select ongoing clinical trials investigating these therapies in addition to other checkpoint inhibitors is shown in Table 1.
Checkpoint inhibitors in HNSCC
| Immunotherapeutic | Target | Select ongoing trials |
|---|---|---|
| Pembrolizumab (Pembro) | PD-1 | NCT03546582 (KEYSTROKE) - SBRT +/- Pembro in recurrent or secondary primary HNSCC
NCT02641093 - Pembro + adjuvant RT or CRT (cisplatin) after surgery in HNSCC NCT02296684 - Neoadjuvant Pembro + SOC (surgery or RT) in high risk HNSCC NCT03765918 - Pembro before surgery and Pembro +/- Cisplatin and RT post-operatively in stage III-IV LA HNSCC |
| Nivolumab (Nivo) | PD-1 | NCT03521570 - IMRT + Nivo for recurrent or second primary HNSCC after prior RT (resectable or eligible for curative re-irradiation)
NCT03576417 - SOC (C/RT) +/- Nivo in HNSCC NCT03247712 - Nivo + RT prior to surgical resection of HNSCC |
| Atezolizumab | PD-L1 | NCT03452137 - Atezolizumab or placebo as adjuvant therapy after definitive local therapy in high-risk LA HNSCC
NCT03708224 - Effect of neoadjuvant Atezolizumab prior to surgical resection in HNSCC NCT03818061 - Atezolizumab + Bevacizumab in recurrent/metastatic previously treated HNSCC |
| Durvalumab | PD-L1 | NCT03212469 - Durvalumab + RT or Durvalumab + Tremelimumab and SBRT in metastatic HNSCC (also includes lung and esophageal tumors)
NCT02997332 (MEDINDUCTION) - Durvalumab + Docetaxel, Cisplatin and 5-FU for LA HNSCC NCT03635164 - Radiotherapy + Durvalumab before surgical resection for HPV negative HNSCC |
| Avelumab | PD-L1 | NCT03498378 - Avelumab, Cetuximab, and Palbociclib in recurrent/metastatic HNSCC
NCT02999087 - Avelumab-cetuximab-radiotherapy vs. SOCs in LA HNSCC NCT03260023 - TG4001 and avelumab in patients with HPV-16 positive recurrent or metastatic malignancies (including OPSCC) |
| Ipilimumab | CTLA-4 | NCT02812524 - Intratumoral injections of ipilimumab prior to surgical resection in HNSCC
NCT03799445 - Ipilimumab, nivolumab, and RT for HPV positive OPSCC |
| Tremelimumab | CTLA-4 | NCT03522584 - Tremelimumab + Durvalumab + hypofractionated RT in recurrent/metastatic HNSCC
NCT03212469 - Durvalumab + RT or Durvalumab + Tremelimumab and SBRT in metastatic HNSCC (also includes lung and esophageal tumors) NCT02551159 (KESTREL) - MEDI 4736 +/- Tremelimumab vs. SOC in recurrent/metastatic HNSCC (active, not recruiting) |
| Relatlimab | Lag-3 | NCT04080804 - Nivolumab +/- Relatlimab or Ipilimumab in head and neck cancer |
Development of novel immunotherapeutics
Despite these encouraging results and updated treatment guidelines, it should be noted that overall response rates to these immunotherapies remains low for HNSCC and ongoing clinical trials are evaluating novel immunotherapeutic strategies [Table 2].
Ongoing clinical trials
| Category of therapy | Trial number (clinicaltrials.gov) - name/description |
|---|---|
| Oncolytic viruses | NCT02626000 (MASTERKEY232/KEYNOTE-137) - Talimogene Laherparepvec + Pembro in recurrent/metastatic HNSCC
NCT00625456 - Safety study of recombinant vaccinia virus to treat refractory solid tumors NCT03740256 - Attenuated vaccinia virus (GL-ONC1) in combination with cisplatin and radiation therapy in locoregionally advanced HNSCC |
| Cancer vaccines | NCT03633110 - Safety, tolerability, immunogenicity, and antitumor activity of GEN-009 adjuvanted vaccine
NCT03548467 - Safety, feasibility, efficacy of multiple dosing with VB10.NEO immunotherapy in patients with LA or metastatic solid tumors NCT02432963 - p53MVA vaccine (modified vaccinia virus ankara vaccine expressing p53) + Pembro in solid tumors after failed prior therapy NCT02955290 - Human EGF-rP64K/montanide ISA 51 vaccine (CIMAvax) + nivolumab in advanced HNSCC and non-small cell lung cancer NCT02544880 - PDE5 inhibition via Tadalafil to enhance anti-tumor mucin 1 (MUC1) vaccine efficacy in patients with HNSCC NCT03946358 - Combination of UCPVax vaccine and Atezolizumab for the treatment of human papillomavirus positive cancers (VolATIL) NCT00021424 - Recombinant fowlpox-TRICOM vaccine therapy in stage IV HNSCC NCT03418480 - Phase I/II vaccine dose escalation study with intradermal injections of HPV anti-CD40 RNA vaccine (HARE-40) in patients with advanced HPV 16 + cancers NCT03260023 - TG4001 and Avelumab in patients with HPV-16 positive recurrent or metastatic malignancies (including OPSCC) NCT00257738-0804 GCC: MAGE-A3/HPV 16 vaccine for squamous cell carcinoma of the head and neck NCT02002182 - DXS 11-001 vaccination prior to robotic surgery, HPV-positive OPSCC |
| Immunomodulatory | NCT03689192 - Arginase-1 peptide vaccine in patients with metastatic solid tumors
NCT02752074 (Keynote-252/ECHO-301) - A phase 3 study of pembrolizumab + epacadostat or placebo in subjects with unresectable or metastatic melanoma NCT02740270 - Phase I/Ib study of GWN323 alone and in combination with PDR001 in patients with advanced malignancies and lymphomas NCT02274155 - Anti-OX40 antibody in head and neck cancer patients |
| T-cell therapy | NCT03578406 - HPV-E6-specific anti-PD1 TCR-T cells in the treatment of HPV-positive NHSCC or cervical cancer |
Oncolytic viruses provide potential for direct tumor cell lysis with further activation of an immune specific response. One of the most promising trials involving oncolytic vaccines in HNSCC to date evaluates the use of pembrolizumab in combination with Talimogene laherparepvec in patients with R/M disease. Final study results are pending, however initial updates suggest at least partial response in some patients (NCT02626000). Additional oncolytic viruses are also under early phase studies (NCT00625456, NCT03740256, NCT01584284).
Vaccinations represent a promising novel therapeutic strategy for various malignancies including HNSCC. Vaccines currently under investigation in HNSCC target patient specific TA (NCT03633110, NCT03548467), or TAs that are expressed in the majority of HNSCC such as mutant p53 (NCT02432963, NCT02955290, NCT02544880, NCT03946358). Additional vaccines are designed to enhance a general immune response such as those using the fowlpox-TRICOM vaccine (NCT00021424). For patients with HPV-mediated disease, the potential for vaccines targeting HPV specific peptides has gained enthusiasm and there are multiple ongoing trials investigating vaccines in this subset (NCT03418480, NCT03260023, NCT00257738, NCT02002182).
Both oncolytic viruses and vaccine therapy aim to promote a tumor specific adaptive immune response. Additional novel therapeutics have also been developed to try to remove the inhibitory signals that suppress an already active immune response.
One example of this strategy is the targeting of MDSCs, as multiple studies have shown these cells to be present in high abundance in HNSCC[38,75]. In vivo studies have shown that elimination of MDSCs from the tumor microenvironment results in decreased Tregs and increased activity of CTLs[76]. As discussed above, Arg, NOS, and IDO are thought to play a role in MDSC mediated Treg function; thus, drugs targeting these pathways are of particular interest. Phosphodiesterase-5 inhibitors are known to reduce both NOS and Arg production and a recent clinical trial leveraged the already FDA approved drug Tadalafil for use in HNSCC. In this randomized, double blinded, placebo controlled trial, patients with previously untreated (primary or recurrent) HNSCC received either tadalafil or placebo for 10 or more days prior to definite treatment. This study revealed decreased MDSC and Treg populations in the tadalafil treated cohort compared to placebo controls as well as increased CTL activity. Subgroup analysis of patients with available tumor specimens (n = 6) demonstrated increased tumor specific immunity in the Tadalafil treated group[37]. No measures of survival outcomes were reported for this study. An additional clinical trial (NCT03689192) evaluating a vaccine targeting arginase is also currently underway.
Inhibition of IDO in combination with Pembrolizumab has also been under intense study in various malignancies[77]. In HNSCC, a phase III clinical trial evaluating IDO inhibitor, Epacadostat in combination with Pembrolizumab (NCT02752074), was unfortunately halted after a similar trial in melanoma revealed no improvement in overall or progression free survival with the addition of Epacadostat to pembrolizumab compared to the control arm[36].
Additional therapies targeting immunosuppressive cytokines have also been developed[78]. Current trials investigating antagonists of TNF receptor aims to inhibit Treg activity and are being tested both as monotherapy and in combination with anti-PD-1 therapies in HNSCC (NCT02740270, NCT02274155).
The final step in the cancer immunity cycle involves tumor cell death induced by activated CTLs. The ideal immunotherapy would bypass the preceding steps and provide T cells already primed to patient specific antigens. This has been successful in hematologic malignancies with therapies such as CAR-T and multiple ongoing clinical trials are investigating the use of T-cell therapies in solid malignancies as well[79]. A clinical trial investigating the use of adoptive T cell transfer in HPV mediated disease in currently ongoing (NCT03578406). A previous study has shown some promise in seven patients with head and neck cancer (5 with SCC, 1 with melanoma and 1 with spindle cell sarcoma)[80].
There are also ongoing trials assessing unique approaches that target multiple aspects of the immune cycle. MVX-ONCO-1 is a treatment that involves subcutaneous injection of capsules containing immune-modulatory granulocyte-macrophage colony stimulating factor and irradiated tumor cells with the aim of stimulating a tumor specific immune response (NCT02999646).
Conclusion
HNSCC represents a diverse group of diseases and exhibits varying degrees of immune dysregulation. Traditional therapeutic approaches are curative in 50% of patients and have proven to have immunomodulatory effects. Currently approved immunotherapies have shown some promise but unfortunately only a small fraction of patients benefit. This review summarizes the most common immune disruptions identified in head and neck cancer and discusses ongoing approaches aimed at targeting the tumor immune microenvironment.
Declarations
Authors’ contributionsConceptualization, data curation, writing, review/editing: Heft Neal ME
Writing, review/editing: Haring CT
Writing, review/editing: Mann JE
Supervision, review/editing: Brenner JC
Conceptualization, writing, review/editing: Spector ME
Conceptualization, writing, review/editing: Swiecicki PL
Availability of data and materialsNot applicable.
Financial support and sponsorshipHeft Neal ME was supported in part by the NIH Grant (T32 DC005356). Brenner JC was supported in part by American Cancer Society Grant: 132034-RSG-18-062-01-TBG. Brenner JC was supported by F31: DE-027600-01.
Conflicts of interestAll authors declared that there are no conflicts of interest.
Ethical approval and consent to participateNot applicable.
Consent for publicationNot applicable.
Copyright© The Author(s) 2019.
REFERENCES
1. Ferlay J, Soerjomataram I, Dikshit R, Eser S, Mathers C, et al. Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 2015;136:E359-86.
2. Chaturvedi AK, Engels EA, Pfeiffer RM, Hernandez BY, Xiao W, et al. Human papillomavirus and rising oropharyngeal cancer incidence in the United States. J Clin Oncol 2011;29:4294-301.
3. Argiris A, Karamouzis MV, Raben D, Ferris RL. Head and neck cancer. Lancet. Lancet 2008;371:1695-709.
4. Forastiere AA, Goepfert H, Maor M, Pajak TF, Weber R, et al. Concurrent chemotherapy and radiotherapy for organ preservation in advanced laryngeal cancer. N Engl J Med 2003;349:2091-8.
5. Taneja C, Allen H, Koness RJ, Radie-Keane K, Wanebo HJ. Changing patterns of failure of head and neck cancer. Arch Otolaryngol Head Neck Surg 2002;128:324-7.
6. Baxi S, Fury M, Ganly I, Rao S, Pfister DG. Ten years of progress in head and neck cancers. J Natl Compr Cancer Netw 2012;10:806-10.
7. Ferris RL, Blumenschein G Jr, Fayette J, Guigay J, Gillison ML. Nivolumab for recurrent squamous-cell carcinoma of the head and neck. N Engl J Med 2016;375:1856-67.
8. Seiwert TY, Burtness B, Mehra R, Weiss J, Berger R, et al. Safety and clinical activity of pembrolizumab for treatment of recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-012): an open-label, multicentre, phase 1b trial. Lancet Oncol 2016;17:956-65.
9. US Food and Drug. FDA approves pembrolizumab for first-line treatment of head and neck squamous cell carcinoma. Available from: https://www.fda.gov/drugs/resources-information-approved-drugs/fda-approves-pembrolizumab-first-line-treatment-head-and-neck-squamous-cell-carcinoma [Last accessed on 12 Nov 2019].
10. Chen DS, Mellman I. Oncology meets immunology: the cancer-immunity cycle. Immunity 2013;39:1-10.
12. Blankenstein T, Coulie PG, Gilboa E, Jaffee EM. The determinants of tumour immunogenicity. Nat Rev Cancer 2012;12:307-13.
13. Champiat S, Ferte C, Lebel-Binay S, Eggermont A, Soria JC. Exomics and immunogenics: bridging mutational load and immune checkpoints efficacy. Oncoimmunology 2014;3:e27817.
14. Lawrence MS, Stojanov P, Polak P, Kryukov GV, Cibulskis K, et al. Mutational heterogeneity in cancer and the search for new cancer-associated genes. Nature 2013;499:214-8.
15. Cannataro VL, Gaffney SG, Sasaki T, Issaeva N, Grewal NKS, et al. APOBEC-induced mutations and their cancer effect size in head and neck squamous cell carcinoma. Oncogene 2019;38:3475-87.
16. Gensterblum-Miller E, Brenner JC. Protecting tumors by preventing human papilloma virus antigen presentation: insights from emerging bioinformatics algorithms. Cancers (Basel) 2019;11:E1543.
17. Sharon H, Pritchard AL. Identifying neoantigens for use in immunotherapy. Mamm Genome 2018;29:714-30.
18. Lee CH, Yelensky R, Jooss K, Chan TA. Update on tumor neoantigens and their utility: why it is good to be Different. Trends Immunol 2018;39:536-48.
19. Soria-Guerra RE, Nieto-Gomez R, Govea-Alonso DO, Rosales-Mendoza S. An overview of bioinformatics tools for epitope prediction: implications on vaccine development. J Biomed Inform 2015;53:405-14.
20. Concha-Benavente F, Srivastava R, Ferrone S, Ferris RL. Immunological and clinical significance of HLA class I antigen processing machinery component defects in malignant cells. Oral Oncol 2016;58:52-8.
21. Ferris RL, Hunt JL, Ferrone S. Human leukocyte antigen (HLA) class I defects in head and neck cancer: molecular mechanisms and clinical significance. Immunol Res 2005;33:113-33.
22. Campo MS, Graham SV, Cortese MS, Ashrafi GH, Araibi EH, et al. HPV-16 E5 down-regulates expression of surface HLA class I and reduces recognition by CD8 T cells. Virology 2010;407:137-42.
23. Cicchini L, Blumhagen RZ, Westrich JA, Myers ME, Warren CJ, et al. High-risk human papillomavirus E7 alters host DNA methylome and represses HLA-E expression in human keratinocytes. Sci Rep 2017;7:3633.
24. de Freitas AC, de Oliveira THA, Barros MR Jr, Venuti A. hrHPV E5 oncoprotein: immune evasion and related immunotherapies. J Exp Clin Cancer Res 2017;36:71.
25. Meissner M, Reichert TE, Kunkel M, Gooding W, Whiteside TL, et al. Defects in the human leukocyte antigen class I antigen processing machinery in head and neck squamous cell carcinoma: association with clinical outcome. Clin Cancer Res 2005;11:2552-60.
26. Ogino T, Shigyo H, Ishii H, Katayama A, Miyokawa N, et al. HLA class I antigen down-regulation in primary laryngeal squamous cell carcinoma lesions as a poor prognostic marker. Cancer Res 2006;66:9281-9.
27. Moy JD, Moskovitz JM, Ferris RL. Biological mechanisms of immune escape and implications for immunotherapy in head and neck squamous cell carcinoma. Eur J Cancer 2017;76:152-66.
28. Rudd CE, Taylor A, Schneider H. CD28 and CTLA-4 coreceptor expression and signal transduction. Immunol Rev 2009;229:12-26.
29. Ariffin AB, Forde PF, Jahangeer S, Soden DM, Hinchion J. Releasing pressure in tumors: what do we know so far and where do we go from here? A review. Cancer Res 2014;74:2655-62.
30. Farsaci B, Donahue RN, Coplin MA, Grenga I, Lepone LM, et al. Immune consequences of decreasing tumor vasculature with antiangiogenic tyrosine kinase inhibitors in combination with therapeutic vaccines. Cancer Immunol Res 2014;2:1090-102.
31. Hamzah J, Jugold M, Kiessling F, Rigby P, Manzur M, et al. Vascular normalization in Rgs5-deficient tumours promotes immune destruction. Nature 2008;453:410-4.
32. Allen CT, Clavijo PE, Van Waes C, Chen Z. Anti-tumor immunity in head and neck cancer: understanding the evidence, how tumors escape and immunotherapeutic approaches. Cancers 2015;7:2397-414.
33. Economopoulou P, Perisanidis C, Giotakis EI, Psyrri A. The emerging role of immunotherapy in head and neck squamous cell carcinoma (HNSCC): anti-tumor immunity and clinical applications. Ann Transl Med 2016;4:173.
34. Fujii N, Shomori K, Shiomi T, Nakabayashi M, Takeda C, et al. Cancer-associated fibroblasts and CD163-positive macrophages in oral squamous cell carcinoma: their clinicopathological and prognostic significance. J Oral Pathol Med 2012;41:444-51.
35. Spanos WC, Hoover A, Harris GF, Wu S, Strand GL, et al. The PDZ binding motif of human papillomavirus type 16 E6 induces PTPN13 loss, which allows anchorage-independent growth and synergizes with ras for invasive growth. J Virol 2008;82:2493-500.
36. Long GV, Dummer R, Hamid O, Gajewski TF, Caglevic C, et al. Epacadostat plus pembrolizumab versus placebo plus pembrolizumab in patients with unresectable or metastatic melanoma (ECHO-301/KEYNOTE-252): a phase 3, randomised, double-blind study. Lancet Oncol 2019;20:1083-97.
37. Califano JA, Khan Z, Noonan KA, Rudraraju L, Zhang Z, et al. Tadalafil augments tumor specific immunity in patients with head and neck squamous cell carcinoma. Clin Cancer Res 2015;21:30-8.
38. Vasquez-Dunddel D, Pan F, Zeng Q, Gorbounov M, Albesiano E, et al. STAT3 regulates arginase-I in myeloid-derived suppressor cells from cancer patients. J Clin Invest 2013;123:1580-9.
39. Hoesli R, Birkeland AC, Rosko AJ, Issa M, Chow KL, et al. Proportion of CD4 and CD8 tumor infiltrating lymphocytes predicts survival in persistent/recurrent laryngeal squamous cell carcinoma. Oral Oncol 2018;77:83-9.
40. Mandal R, Senbabaoglu Y, Desrichard A, Havel JJ, Dalin MG, et al. The head and neck cancer immune landscape and its immunotherapeutic implications. JCI Insight 2016;1:e89829.
41. Ono T, Azuma K, Kawahara A, Sasada T, Hattori S, et al. Association between PD-L1 expression combined with tumor-infiltrating lymphocytes and the prognosis of patients with advanced hypopharyngeal squamous cell carcinoma. Oncotarget 2017;8:92699-714.
42. Young MR, Wright MA, Lozano Y, Prechel MM, Benefield J, et al. Increased recurrence and metastasis in patients whose primary head and neck squamous cell carcinomas secreted granulocyte-macrophage colony-stimulating factor and contained CD34+ natural suppressor cells. Int J Cancer 1997;74:69-74.
43. Chen L. Co-inhibitory molecules of the B7-CD28 family in the control of T-cell immunity. Nat Rev Immunol 2004;4:336-47.
44. Diamond MS, Kinder M, Matsushita H, Mashayekhi M, Dunn GP, et al. Type I interferon is selectively required by dendritic cells for immune rejection of tumors. J Exp Med 2011;208:1989-2003.
45. Fuertes MB, Kacha AK, Kline J, Woo SR, Kranz DM, et al. Host type I IFN signals are required for antitumor CD8+ T cell responses through CD8 {alpha}+ dendritic cells. J Exp Med 2011;208:2005-16.
46. Zandberg DP, Strome SE. The role of the PD-L1:PD-1 pathway in squamous cell carcinoma of the head and neck. Oral Oncol 2014;50:627-32.
47. Zou W, Wolchok JD, Chen L. PD-L1 (B7-H1) and PD-1 pathway blockade for cancer therapy: mechanisms, response biomarkers, and combinations. Sci Transl Med 2016;8:328.
48. Chen L, Han X. Anti-PD-1/PD-L1 therapy of human cancer: past, present, and future. J Clin Invest 2015;125:3384-91.
49. Badoual C, Hans S, Merillon N, Van Ryswick C, Ravel P, et al. PD-1-expressing tumor-infiltrating T cells are a favorable prognostic biomarker in HPV-associated head and neck cancer. Cancer Res 2013;73:128-38.
50. Lyford-Pike S, Peng S, Young GD, Taube JM, Westra WH, et al. Evidence for a role of the PD-1:PD-L1 pathway in immune resistance of HPV-associated head and neck squamous cell carcinoma. Cancer Res 2013;73:1733-41.
51. Ukpo OC, Thorstad WL, Lewis JS Jr. B7-H1 expression model for immune evasion in human papillomavirus-related oropharyngeal squamous cell carcinoma. Head Neck Pathol 2013;7:113-21.
52. Tran L, Allen CT, Xiao R, Moore E, Davis R, et al. Cisplatin alters antitumor immunity and synergizes with PD-1/PD-L1 inhibition in head and neck squamous cell carcinoma. Cancer Immunol Res 2017;5:1141-51.
53. de Biasi AR, Villena-Vargas J, Adusumilli PS. Cisplatin-induced antitumor immunomodulation: a review of preclinical and clinical evidence. Clin Cancer Res 2014;20:5384-91.
54. Hato SV, Khong A, de Vries IJ, Lesterhuis WJ. Molecular pathways: the immunogenic effects of platinum-based chemotherapeutics. Clin Cancer Res 2014;20:2831-7.
55. Reits EA, Hodge JW, Herberts CA, Groothuis TA, Chakraborty M, et al. Radiation modulates the peptide repertoire, enhances MHC class I expression, and induces successful antitumor immunotherapy. J Exp Med 2006;203:1259-71.
56. Klein B, Loven D, Lurie H, Rakowsky E, Nyska A, et al. The effect of irradiation on expression of HLA class I antigens in human brain tumors in culture. J Neurosurg 1994;80:1074-7.
57. Santin AD, Hiserodt JC, Fruehauf J, DiSaia PJ, Pecorelli S, et al. Effects of irradiation on the expression of surface antigens in human ovarian cancer. Gynecol Oncol 1996;60:468-74.
58. Santin AD, Rose GS, Hiserodt JC, Fruehauf J, Eck LM, et al. Effects of cytokines combined with high-dose gamma irradiation on the expression of major histocompatibility complex molecules and intercellular adhesion molecule-1 in human ovarian cancers. Int J Cancer 1996;65:688-94.
59. Lugade AA, Moran JP, Gerber SA, Rose RC, Frelinger JG, et al. Local radiation therapy of B16 melanoma tumors increases the generation of tumor antigen-specific effector cells that traffic to the tumor. J Immunol 2005;174:7516-23.
60. Manukian G, Bar-Ad V, Lu B, Argiris A, Johnson JM. Combining radiation and immune checkpoint blockade in the treatment of head and neck squamous cell carcinoma. Front Oncol 2019;9:122.
61. Abuodeh Y, Venkat P, Kim S. Systematic review of case reports on the abscopal effect. Curr Probl Cancer 2016;40:25-37.
62. Postow MA, Callahan MK, Barker CA, Yamada Y, Yuan J, et al. Immunologic correlates of the abscopal effect in a patient with melanoma. New Engl J Med 2012;366:925-31.
63. Jie HB, Schuler PJ, Lee SC, Srivastava RM, Argiris A, et al. CTLA-4(+) regulatory T cells increased in cetuximab-treated head and neck cancer patients suppress NK cell cytotoxicity and correlate with poor prognosis. Cancer Res 2015;75:2200-10.
64. Concha-Benavente F, Srivastava RM, Trivedi S, Lei Y, Chandran U, et al. Identification of the cell-intrinsic and -extrinsic pathways downstream of EGFR and IFNgamma that induce PD-L1 expression in head and neck cancer. Cancer Res 2016;76:1031-43.
65. Pahl JH, Ruslan SE, Buddingh EP, Santos SJ, Szuhai K, et al. Anti-EGFR antibody cetuximab enhances the cytolytic activity of natural killer cells toward osteosarcoma. Clin Cancer Res 2012;18:432-41.
66. Lee J, Moon C. Current status of experimental therapeutics for head and neck cancer. Exp Biol Med 2011;236:375-89.
67. Roberti MP, Barrio MM, Bravo AI, Rocca YS, Arriaga JM, et al. IL-15 and IL-2 increase cetuximab-mediated cellular cytotoxicity against triple negative breast cancer cell lines expressing EGFR. Breast Cancer Res Treat 2011;130:465-75.
68. Hsu YF, Ajona D, Corrales L, Lopez-Picazo JM, Gurpide A, et al. Complement activation mediates cetuximab inhibition of non-small cell lung cancer tumor growth in vivo. Mol Cancer 2010;9:139.
69. Srivastava RM, Lee SC, Andrade Filho PA, Lord CA, Jie HB, et al. Cetuximab-activated natural killer and dendritic cells collaborate to trigger tumor antigen-specific T-cell immunity in head and neck cancer patients. Clin Cancer Res 2013;19:1858-72.
70. Cohen EEW, Soulieres D, Le Tourneau C, Dinis J, Licitra L, et al. Pembrolizumab versus methotrexate, docetaxel, or cetuximab for recurrent or metastatic head-and-neck squamous cell carcinoma (KEYNOTE-040): a randomised, open-label, phase 3 study. Lancet 2019;393:156-67.
71. Rischin D, Harrington KJ, Greil R, Soulieres D, Tahara M, et al. Protocol-specified final analysis of the phase 3 KEYNOTE-048 trial of pembrolizumab (pembro) as first-line therapy for recurrent/metastatic head and neck squamous cell carcinoma (R/M HNSCC). J Clin Oncol 2019;37:6000.
72. Colevas AD, Bahleda R, Braiteh F, Balmanoukian A, Brana I, et al. Safety and clinical activity of atezolizumab in head and neck cancer: results from a phase I trial. Ann Oncol 2018;29:2247-53.
73. Segal NH, Ou SI, Balmanoukian A, Fury MG, Massarelli E, et al. Safety and efficacy of durvalumab in patients with head and neck squamous cell carcinoma: results from a phase I/II expansion cohort. Eur J Cancer 2019;109:154-61.
74. Licitra LF, Haddad RI, Even C, Tahara M, Dvorkin M, et al. EAGLE: a phase 3, randomized, open-label study of durvalumab (D) with or without tremelimumab (T) in patients (pts) with recurrent or metastatic head and neck squamous cell carcinoma (R/M HNSCC). J Clin Oncol 2019;37:6012.
75. Pak AS, Wright MA, Matthews JP, Collins SL, Petruzzelli GJ, et al. Mechanisms of immune suppression in patients with head and neck cancer: presence of CD34(+) cells which suppress immune functions within cancers that secrete granulocyte-macrophage colony-stimulating factor. Clin Cancer Res 1995;1:95-103.
76. Serafini P, Meckel K, Kelso M, Noonan K, Califano J, et al. Phosphodiesterase-5 inhibition augments endogenous antitumor immunity by reducing myeloid-derived suppressor cell function. J Exp Med 2006;203:2691-702.
77. Komiya T, Huang CH. Updates in the clinical development of epacadostat and other indoleamine 2,3-dioxygenase 1 inhibitors (IDO1) for human cancers. Front Oncol 2018;8:423.
78. Gadhikar MA, Myers JN. Recent advances in head and neck cancer: the beginning of the immunotherapy era in HNSCC. Adv Mod Oncol Res 2018;4.
79. Newick K, O’Brien S, Moon E, Albelda SM. CAR T cell therapy for solid tumors. Ann Rev Med 2017;68:139-52.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Neal MEH, Haring CT, Mann JE, Brenner JC, Spector ME, Swiecicki PL. Novel immunotherapeutic approaches in head and neck cancer. J Cancer Metastasis Treat 2019;5:76. http://dx.doi.org/10.20517/2394-4722.2019.32
AMA Style
Neal MEH, Haring CT, Mann JE, Brenner JC, Spector ME, Swiecicki PL. Novel immunotherapeutic approaches in head and neck cancer. Journal of Cancer Metastasis and Treatment. 2019; 5: 76. http://dx.doi.org/10.20517/2394-4722.2019.32
Chicago/Turabian Style
Neal, Molly E. Heft, Catherine T. Haring, Jacqueline E. Mann, J. Chad Brenner, Matthew E. Spector, Paul L. Swiecicki. 2019. "Novel immunotherapeutic approaches in head and neck cancer" Journal of Cancer Metastasis and Treatment. 5: 76. http://dx.doi.org/10.20517/2394-4722.2019.32
ACS Style
Neal, MEH.; Haring CT.; Mann JE.; Brenner JC.; Spector ME.; Swiecicki PL. Novel immunotherapeutic approaches in head and neck cancer. J. Cancer. Metastasis. Treat. 2019, 5, 76. http://dx.doi.org/10.20517/2394-4722.2019.32
About This Article
Special Issue
Copyright
Data & Comments
Data
 Cite This Article 12 clicks
Cite This Article 12 clicks











Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.